Bloodborne pathogens that can cause serious or fatal infections are a major risk to employees, especially in the healthcare industry. To protect workers from pathogens and instruments that come in contact with them, they must be disposed of properly in biosafety containers. Biosafety, also called sharps containers are commonly constructed with rigid plastic material and colored red with a biohazard label. The Occupational Safety and Health Administration (OSHA) defines a contaminated sharp as “any contaminated object that can penetrate the skin including, but not limited to, needles, scalpels, broken glass, broken capillary tubes, and exposed ends of dental wires.”In this blog, we will explore the significance of biosafety containers, their design, regulatory guidelines, disposal procedures, training, and the responsibility of healthcare workers in promoting biosafety practices.

The Risk of Bloodborne Pathogens
Bloodborne pathogens pose a significant risk to healthcare workers, making it crucial to understand their potential dangers. In this section, we will explore the types of bloodborne pathogens that can cause serious or fatal infections and the impact they have on employee safety, particularly in the healthcare industry.
Types of Bloodborne Pathogens:
- Hepatitis B Virus (HBV): HBV is a highly contagious virus that can cause chronic liver disease and increase the risk of liver cancer.
- Hepatitis C Virus (HCV): HCV can lead to chronic liver disease and is a leading cause of liver transplants.
- Human Immunodeficiency Virus (HIV): HIV attacks the immune system, leading to acquired immunodeficiency syndrome (AIDS) and making individuals more susceptible to various infections and diseases.
Also Read: Templates Bloodborne Pathogens and BBP Exposure control Plan
Modes of Transmission:
- Direct Contact: Bloodborne pathogens can be transmitted through direct contact with infected blood or bodily fluids. This can occur through needlestick injuries, cuts, or contact with mucous membranes or non-intact skin.
- Contaminated Sharps: Improper disposal of contaminated sharps, such as needles and scalpels, can result in accidental injuries and transmission of bloodborne pathogens.
- Exposure to Other Body Fluids: Pathogens can also be present in other body fluids, including semen, vaginal secretions, and cerebrospinal fluid, posing a risk of transmission if proper precautions are not taken.
Risks to Healthcare Workers:
- Needlestick Injuries: Healthcare workers, including nurses, doctors, and laboratory personnel, are at high risk of needlestick injuries, which can lead to immediate infection with bloodborne pathogens.
- Occupational Exposure: Healthcare settings often involve handling blood and bodily fluids, increasing the potential for exposure to bloodborne pathogens.
- Long-Term Health Consequences: Infections caused by bloodborne pathogens can have severe long-term health implications, including chronic liver disease, compromised immune systems, and increased risk of certain cancers.
Impact on Employee Safety:
- Emotional and Psychological Stress: The fear of contracting bloodborne infections can lead to significant emotional and psychological stress among healthcare workers.
- Occupational Health and Safety: Bloodborne pathogens pose a threat to the occupational health and safety of healthcare workers, highlighting the need for appropriate preventative measures.
- Legal and Ethical Considerations: Employers have a legal and ethical obligation to provide a safe working environment and protect employees from bloodborne pathogens.
Design and Construction of Biosafety Containers
In this section, we will explore the design and construction of biosafety containers, focusing on the materials used, their distinctive features, and the importance of visual indicators for effective use.

- Materials Used in Biosafety Container Construction:
- Rigid Plastic: Biosafety containers are typically constructed using rigid plastic materials such as polypropylene or high-density polyethene. These materials provide durability and resistance to punctures, ensuring the containment of sharps and preventing accidental injuries.
- Leak-Resistant Properties: Biosafety containers are designed to be leak-resistant, reducing the risk of blood or other potentially infectious materials seeping out of the container.
- Puncture-Proof Design: The construction of biosafety containers incorporates features that minimize the risk of sharps penetrating the container, further enhancing safety.
- Distinctive Features of Biosafety Containers:
- Red Color: Biosafety containers are commonly coloured red, which serves as a visual indicator to distinguish them from regular waste containers. The red colour alerts healthcare workers and others to the potential presence of hazardous materials.
- Biohazard Label: A prominent biohazard label is affixed to the container, clearly indicating its purpose and warning individuals of the potential risks associated with its contents.
- Sealing Mechanism: Biosafety containers are equipped with secure, tamper-proof sealing mechanisms to prevent accidental spills and ensure the safe containment of sharps.
- Different Sizes and Types of Biosafety Containers:
- Variety of Sizes: Biosafety containers are available in various sizes to accommodate different healthcare settings and disposal needs. They range from small, portable containers used in patient rooms to larger containers used in clinical laboratories or operating rooms.
- Wall-Mounted Options: Some biosafety containers are designed to be wall-mounted, allowing for convenient placement in areas where sharps disposal is frequently required.
- Travel-Friendly Containers: Specialized biosafety containers are available for travel purposes, ensuring safe sharps disposal outside of healthcare facilities.
- Compliance with Regulatory Guidelines:
- Regulatory Standards: Biosafety containers must meet specific regulatory guidelines and standards set by organizations such as the Occupational Safety and Health Administration (OSHA) and the Centers for Disease Control and Prevention (CDC). These standards ensure the effectiveness and safety of the containers.
- Disposal Regulations: Proper disposal of biosafety containers, including the container itself when full, must adhere to local, state, and federal regulations governing biohazardous waste management.
Regulatory Guidelines and Standards:
- Occupational Safety and Health Administration (OSHA):
- OSHA’s Bloodborne Pathogens Standard (29 CFR 1910.1030) sets guidelines for the safe handling and disposal of blood and other potentially infectious materials.
- The standard mandates the use of appropriate containers, such as biosafety containers, for the disposal of contaminated sharps.
- OSHA regulations also cover training requirements for healthcare workers regarding sharps disposal and the use of biosafety containers.
- Centres for Disease Control and Prevention (CDC):
- The CDC provides guidelines for infection control in healthcare settings, including recommendations for sharps disposal.
- The CDC’s guidance emphasizes the use of puncture-resistant and leak-proof containers, such as biosafety containers, for the safe disposal of contaminated sharps.
- These guidelines also offer recommendations for the placement, accessibility, and labelling of biosafety containers in healthcare facilities.
Proper Disposal Procedures:
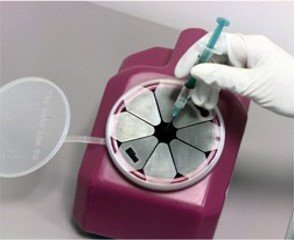
- Segregation and Containment:
- Sharps waste should be segregated from other types of medical waste to prevent accidental injuries.
- Contaminated sharps should be immediately placed in a designated biosafety container to ensure safe containment.
- Safe Handling and Transportation:
- Healthcare workers should handle biosafety containers with caution, using appropriate personal protective equipment (PPE) to minimize the risk of exposure.
- Containers should be securely closed and transported to the appropriate disposal area using designated carts or trolleys.
- Disposal Methods and Facilities:
- Biosafety containers should be disposed of according to local, state, and federal regulations governing biohazardous waste management.
- Disposal methods may include incineration, autoclaving, or other approved methods to ensure the complete destruction of infectious materials.
- Healthcare facilities should have designated areas or contracts with licensed waste management companies for the proper disposal of biohazardous waste.
Also Read:
Training and Education:
- Healthcare Worker Training:
- Healthcare workers should receive comprehensive training on proper sharps disposal practices, including the use of biosafety containers.
- Training programs should cover the identification of contaminated sharps, the selection and use of appropriate containers, and safe handling techniques.
- Ongoing Education and Updates:
- Regular education and training sessions should be conducted to keep healthcare workers updated on regulatory guidelines, best practices, and any changes in biosafety container requirements.
- Training should also address the importance of reporting incidents and near misses related to sharps disposal to improve safety protocols.
- Collaboration with Management:
- Healthcare facilities should foster a culture of safety by collaborating with management to ensure adequate resources, training opportunities, and compliance with biosafety practices.
- Management should support and encourage open communication regarding biosafety concerns and provide feedback to continuously improve sharps disposal protocols.
Read More: Bloodborn Pathogens Training Materials
Biosafety Containers Safety Facts

- Provide easy access to sharps containers and keep them in areas where sharps are used.
- Never open or empty sharps containers.
- Maintain sharps containers in an upright position, replace them on a routine basis, close them when moving, and do not overfill them.
- Sort, handle, transport, or ship-regulated waste in containers constructed to prevent leakage.
- Watch out for any sharp object when picking up regular trash. Always carry full trash bags away from your body to avoid being stuck by hidden sharps hazards.
- Do not push trash down into the trash bag to avoid being stuck by hidden hazards.
- Never pick up contaminated broken glass, even with gloved hands; use tongs, forceps, or a brush and dust-pan.
- If you are accidentally stuck with sharps, im- mediately wash the affected area with soap and running water for approximately 10 minutes.
- Report any injury caused by sharps to your super- visor as soon as possible.
- Dispose of all regulated waste according to federal, state, and local regulations.
Conclusion
In conclusion, biosafety containers play a critical role in protecting healthcare workers from the risk of bloodborne pathogens. By providing a safe and designated means of disposing of contaminated sharps, biosafety containers contribute to maintaining a healthy and secure environment in healthcare settings. Adhering to regulatory guidelines, implementing proper disposal procedures, investing in training and education, and fostering a culture of biosafety are key steps in ensuring the effectiveness of biosafety containers. By prioritizing worker safety and following best practices, we can mitigate the risks associated with bloodborne pathogens and create a safer working environment for healthcare professionals.
Also Read: Managing Risk In Healthcare
For more safety Resources Please Visit Safetybagresources